Introdução
Nighttime leg cramps are sudden, intense muscle contractions that frequently disrupt sleep in older adults. Typically affecting the calves, hamstrings, and sometimes the feet, these cramps can last from seconds to several minutes and leave residual stiffness or soreness. Age-related changes in muscle composition, neuromuscular control, dehydration, and electrolyte imbalances are common contributing factors. CO₂ cryotherapy has emerged as a targeted, non-invasive therapy that may reduce cramp frequency and improve muscle comfort. This article explores the mechanisms of nighttime leg cramps, the role of CO₂ cryotherapy, current research evidence, and practical strategies for seniors to integrate cryotherapy into a broader muscle health regimen.
1. Understanding Nighttime Leg Cramps in Seniors
1.1 What Are Nighttime Leg Cramps?
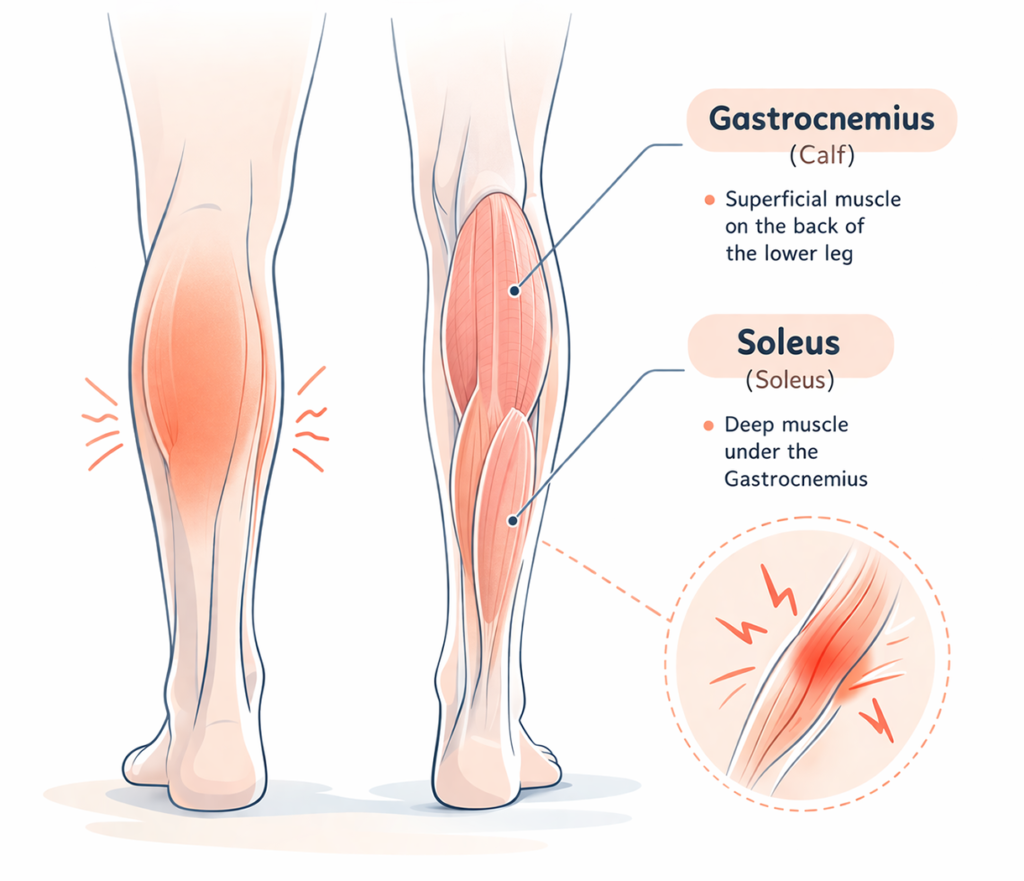
Nighttime leg cramps are involuntary, painful contractions of skeletal muscles occurring during rest or sleep. The gastrocnemius and soleus muscles are most commonly affected. These cramps may wake individuals abruptly and can leave persistent tension or soreness in the muscle. Clinically, these episodes are referred to as “nocturnal skeletal muscle cramps” and are distinct from restless leg syndrome or periodic limb movement disorders. Differentiating these conditions is crucial for targeting interventions toward muscle physiology rather than general neurological modulation.
1.2 Why Seniors Are More Susceptible
Aging leads to sarcopenia, a reduction in muscle mass and strength, making muscles more prone to fatigue. Neuromuscular control diminishes, reducing coordination between nerves and muscle fibers. Electrolyte imbalances—particularly low magnesium, potassium, and calcium—are common due to dietary insufficiencies, medications, and underlying health conditions. Additionally, chronic illnesses such as diabetes and peripheral vascular disease further compromise muscle metabolism and microcirculation, increasing the likelihood and severity of cramps.
1.3 Common Triggers and Patterns
Prolonged immobility, dehydration, extended periods of standing during the day, or positional changes during sleep can precipitate cramps. Electrolyte disturbances destabilize muscle membrane potentials, heightening excitability. Certain medications, such as diuretics and statins, and stimulants like caffeine, may further increase susceptibility. Identifying these triggers is critical for designing prevention strategies that complement therapies such as cryotherapy.
2. CO₂ Cryotherapy: A Targeted Approach
2.1 What Is CO₂ Cryotherapy?
CO₂ cryotherapy involves the local application of carbon dioxide gas at controlled low temperatures to specific muscles or joints. Unlike whole-body cryotherapy, CO₂ therapy focuses on localized tissue cooling. Cold exposure induces initial vasoconstriction followed by reactive vasodilation, improving microcirculation and reducing localized inflammation. The therapy leverages physiological responses to cold to modulate tissue metabolism, blood flow, and neural signaling.
2.2 Mechanisms of Muscle Relief
Cryotherapy reduces nerve conduction velocity, dampening pain signals from affected muscles. It lowers tissue metabolic demand, limiting secondary inflammation. Reactive vasodilation following vasoconstriction improves oxygen and nutrient delivery, facilitating muscle recovery and reducing stiffness. CO₂ therapy targets nociceptors and improves circulation, potentially decreasing both the severity and frequency of nighttime cramps in older adults.
2.3 Advantages Over Traditional Ice Therapy
Traditional ice packs provide inconsistent cooling, short-duration effects, and risk of frostbite. CO₂ cryotherapy offers precise temperature control and deeper tissue penetration, making it safer for older adults with fragile skin. Its uniform cooling effect ensures more consistent physiological responses, making CO₂ therapy a highly effective alternative for localized muscle relief.
3. Physiological Mechanisms of CO₂ Cryotherapy
3.1 Microcirculation Enhancement
Microcirculation involves the smallest blood vessels that deliver oxygen and nutrients to muscles. Aging often impairs these systems, slowing waste clearance and increasing cramp risk. CO₂ cryotherapy triggers a biphasic vascular response—initial vasoconstriction followed by vasodilation—which enhances blood flow, supports tissue recovery, and mitigates metabolic imbalance that contributes to cramps.
3.2 Neuromuscular Modulation
Cramps are caused by involuntary firing of motor units. CO₂ cryotherapy reduces nerve conduction velocity, interrupting abnormal motor signals. By modulating neuromuscular excitability, therapy decreases both cramp intensity and frequency.
3.3 Anti-inflammatory Effects
Muscle microtrauma or overuse induces inflammation, increasing soreness and susceptibility to cramps. Cryotherapy reduces pro-inflammatory cytokines while promoting anti-inflammatory pathways, aiding recovery and enhancing muscle resilience.
4. Research Evidence
4.1 Clinical Studies on Muscle Pain
Localized cryotherapy has demonstrated effectiveness in reducing muscle pain and improving function in clinical studies. While research specific to nighttime leg cramps in seniors is limited, studies on post-exercise and injury-induced muscle pain support the concept that controlled cooling alleviates discomfort, providing a rationale for nighttime cramp management.
4.2 Comparative Effectiveness
Compared to heat therapy, massage, and electrical stimulation, cryotherapy is particularly effective under inflammatory or hyperexcitable neural conditions. CO₂ cryotherapy’s precise temperature and deep penetration differentiate it from traditional cold applications, delivering consistent physiological responses, especially in older adults with fragile tissues.
4.3 Emerging Research in Aging Populations
Recent studies focus on elderly muscle recovery, microvascular function, and neuromuscular responses. Evidence suggests controlled cryotherapy may help maintain muscle homeostasis and mitigate discomfort associated with aging, offering potential benefit for nighttime cramp prevention.
5. Practical Applications
5.1 Optimal Timing
Cryotherapy can be applied proactively before sleep to reduce muscle excitability or reactively after a cramp to relieve residual discomfort. Short sessions targeting calf muscles are most effective when timed to align with high-risk periods.
5.2 Lifestyle Integration
Hydration, balanced electrolytes, gentle stretching, and low-intensity exercise complement cryotherapy. Addressing underlying health conditions such as diabetes or vascular disease enhances overall muscle health and supports the efficacy of cold therapy.
5.3 Safety Considerations
Seniors with fragile skin, neuropathy, or compromised circulation require careful temperature control. Devices should prevent direct exposure to extreme cold, and medical consultation is advised for those with cardiovascular or severe circulatory disorders.
6. Integrating CO₂ Cryotherapy into Comprehensive Muscle Health Management
6.1 Complementary Exercise Strategies
Cryotherapy should be integrated with regular, low-impact exercise programs that strengthen calf, hamstring, and foot muscles. Strengthened musculature supports joint stability and reduces cramp susceptibility. Combining cryotherapy with resistance training, gentle stretching, and balance exercises creates synergistic benefits for overall muscle resilience.
6.2 Nutritional and Hydration Considerations
Maintaining proper hydration and electrolyte balance—including magnesium, potassium, and calcium—is essential to complement the neuromuscular benefits of cryotherapy. Dietary strategies combined with cold therapy help stabilize membrane excitability in muscle fibers, decreasing spontaneous contractions that cause cramps.
6.3 Preventive and Long-term Benefits
Regular use of CO₂ cryotherapy as part of a broader muscle health plan may reduce the overall frequency and intensity of nighttime cramps over time. By supporting microcirculation, modulating neural excitability, and promoting recovery, cryotherapy acts synergistically with exercise, nutrition, and lifestyle interventions, enhancing sleep quality and daily functional mobility for older adults.
PERGUNTAS FREQUENTES
Can CO₂ cryotherapy completely eliminate nighttime leg cramps?
No, but it significantly reduces frequency and intensity when combined with lifestyle strategies.
Is it safe for seniors with circulation issues?
Yes, but consultation with a healthcare professional is recommended for severe vascular or neuropathic conditions.
How quickly does cryotherapy work?
Most users experience relief within minutes, though responses vary.
Can it be used nightly?
Controlled, short-duration applications are generally safe for daily use.
Does it replace medical management?
No, cryotherapy is an adjunct therapy and should complement standard medical care.
Conclusão
Nighttime leg cramps can significantly disrupt sleep and reduce quality of life in older adults. CO₂ cryotherapy offers a non-invasive method to improve muscle comfort, enhance microcirculation, and modulate neuromuscular activity. When integrated with exercise, nutrition, and healthy lifestyle habits, it becomes a valuable component of comprehensive muscle health management, helping seniors reduce cramp frequency, improve sleep, and maintain functional mobility.
Referências
Miller, K.J. et al. Muscle Cramps: Pathophysiology and Clinical Strategies. Journal of Geriatric Medicine and Aging.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5123867/
Knight, K.L. & Draper, D.O. Therapeutic Modalities: The Art and Science.
https://www.therapeuticmodalitiesbook.com
Bleakley, C.M., et al. The Use of Cryotherapy in Inflammation and Recovery. Journal of Athletic Training.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2951296/
Ihsan, M., et al. Physiological Mechanisms of Cooling in Muscle Recovery. Sports Medicine.
https://link.springer.com/article/10.1007/s40279-016-0533-8
Local Cryotherapy Official Website. CO₂ Cryotherapy for Muscle and Joint Comfort.


